Sexual Education & Healthcare: Barriers for Women with Spina Bifida
- Jul 3, 2021
- 6 min read
Updated: Oct 24, 2021
By: Jules Ferguson
For this article, we will primarily be referencing a research study done by Streur et al., (2019). The aim of this study was to determine what women with spina bifida understand about their sexual health, how they learned about it, what questions they have, and their experiences with their sexuality.
What is Spina Bifida?
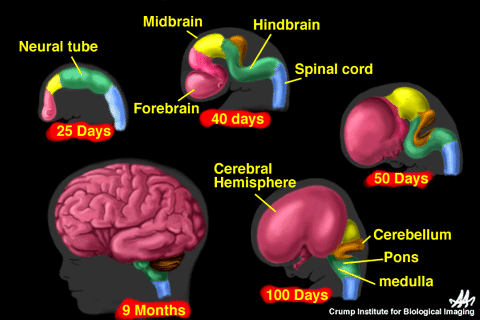
Women with disabilities face many restrictions when accessing sexual healthcare, and patients with spina bifida (SB) are no exception (1). Spina bifida occurs during the early stages of pregnancy, where the neural tube (early stage of spinal cord and brain) of the fetus does not develop as expected (3).
This can result in abnormalities in the spine and spinal cord. The condition can be caused by either genetic, dietary, or environmental during pregnancy, but most attest the condition to a lack of folic acid from diet during pregnancy.
There are two main types of SB: Oculta and Myelomeningocele. Spina Bifida occulta often has less severe symptoms because the spinal nerves are less affected. Myelomeningocele is often more severe because the spinal cord may protrude, the spinal canal may remain open, and tissues and nerves may be exposed. Some people with SB may:
lack sensation
not be able to walk (thus requiring mobility aids such as walkers, crutches, or wheelchairs)
experience bladder or bowel incontinence
Only 5% of women with spina bifida speak about sex with their doctor, yet 55% are sexually active, and 92% hope to have a sexual partner at some point in their life. Without reliable sex education and health resources, they are vulnerable to misconceptions, coercion, and sexual abuse.

Why are individuals with spina bifida perceived as being asexual?
Individuals with SB experience restrictions when accessing sexual healthcare as they are often viewed as asexual individuals by providers. This hinder their access to SB-specific information about their sexual health. Additionally, they often feel as though potential partners do not view them as sexual beings. According to this particular study conducted in 2019, participants mentioned the following:
“…I don’t think that men look at me and think I’m pretty… I always worry when a guy sees me is he seeing me or is he seeing my chair?”
- a 36 year old participant
“I made an appointment with just some random doctor… and he said, ‘so why are you here?’ And I said, ‘for birth control.’ And he’s like, ‘but what do you mean?’ And I was like, ‘well, because I don’t like having babies, like I’m on a college track…’ ‘But like, you’re in a wheelchair.’ And I was like, ‘yeah…’ And he’s like, ‘you can’t stand.’ And I was like, ‘do you stand when you have sex?’”
- a 29 year old participant
How does asexual perception affect sexual healthcare access?
Many people rely on physicians, nurses, and other healthcare providers for information about their health. Women with SB often find themselves restricted when accessing sexual healthcare for many reasons:
Their doctors rarely initiate conversations about reproductive health. If they did, it was focused on menstruation rather than sexual activity.
Many women felt that physicians assumed they were not sexually active and that they were seen as asexual. They are less likely to get pap smears and use birth control than abled-bodied peers.
When patients with SB do discuss sexual health with their doctor, it is almost exclusively prompted by the patient.
Because many patients may feel uncomfortable or unsafe bringing up sexual health, they may not receive the care that they need or may have misconceptions about their health that remain unchecked.
How can SB affect intimate relationships & mental health?
Problems with being seen as asexual were not limited to the doctor's office, as many women expressed that they struggle with finding partners who see them as sexual beings. This stigma can be emotionally challenging, and it can often manifest as poor self-confidence, mental health issues and loneliness.
Women with SB face challenges unique to their sexuality due to: limited mobility, continence, and pain. This can manifest as poor self-image and anxiety, and can often make intimate relationships stressful or complex. Women with SB frequently compared themselves to able-bodied women and felt physically insecure.
Many women with SB have to be mindful of positioning and activity because of hip/back pain. They may also have to consider conditions like vaginal prolapse and diminished sensation. Many must use the bathroom beforehand, limiting their ability to be spontaneous.
Though many women with SB experience anxiety about sex or insecurities, those with supportive and committed partners have less anxiety and greater confidence.
Many women report that their poor confidence and their desire to been seen as sexual beings leave them vulnerable to sexual abuse and coercion. Some tolerated it because they want to be viewed as desirable or loved.
Women are 4X more likely to experience sexual assault if they have a disability, and are more likely to experience coercion or unwanted contact. By recognizing these patterns, healthcare providers, families, and friends can support women with SB and ensure that they are provided with adequate information about healthy relationships and resources to leave unsafe environments.
Where are there shortcomings in sex education for women with Spina Bifida?
Sex education can be challenging for many, and most people will encounter some restrictions when seeking information about their sexuality. Many women are unsure if their public sexual education applied to them and how their disability would affect their sexuality. Why is that?
Women reported that what they were taught in school was often misaligned with what they learned from lived experience.
People with SB receive an average amount of general sex education, but lack SB-specific knowledge about intimacy. They often have questions that are unanswered by their physicians.
74% reported their knowledge of sexual safety with spina bifida was poor or extremely poor.
Many women were unsure about whether they could get STIs, become pregnant, or have any type of sex safely.
As a result some struggle with dangerous misconceptions, fears and unanswered questions about their sexual health.
Why should you care about this research?
There is a scarcity of research focused on sexuality not only in spina bifida patients but throughout the disabled community in general. Women with disabilities are vastly underrepresented in sexuality research and little is known how a woman’s physical experiences influence her self-perception and interpersonal relationships when she has SB.
Most Spina Bifida research in sexuality is focused on men, which may cause further misconceptions among the public and physicians. Streur's research is a critical step into investigating the limitations of the healthcare system when providing sexual health services by primarily focusing on the patients, not the physicians.
Things to consider about Streur's research!
While this research is indeed valuable, we always need to consider the limitations of the articles we read. All scientific information has the potential for bias or gaps in information. An easy way to critically analyze scientific papers is by looking carefully at its methodology. Questions to ask might be: What is the sample size and is it large enough to be generalizable? Who are the participants? Are we asking the right questions during surveys/questionnaires? Keeping that in mind, here are a few things to consider about Streur's research:
The participant group was small (25 women) and only consisted of cisgender women. All but one of the participants identified as heterosexual and most of them defined sex exclusively as penetrative sex. These results may not represent all women with SB, especially queer individuals.
All participants were recruited through healthcare providers at the University of Michigan, meaning that everyone who was surveyed was already accessing healthcare. This indicates that these results may not be representative of people who are unable to see a doctor, for many reasons, such as being unhoused, undocumented, or uninsured.
This does not mean that this research is not valuable. In fact, it indicates the opposite! While this paper has raised awareness for the barriers faced by this underrepresented population, it may also draw attention to other populations who are still not represented in sexuality and health research.
Clinical Implications
Physicians: Please ask your patients about their sexual activity and health. It is your responsibility to initiate these conversations and people with SB should not be treated unfairly because of their disability. If you are concerned about being asked a question you can not answer, that's okay. Take the time to look into SB-specific sexual health information, especially if you know that you have patients with SB or specialize in women's health, urology, sexual health, etc.
Sources:
1. Paper title: “If Everyone Else Is Having This Talk With Their Doctor, Why Am I Not Having This Talk With Mine?”: The Experiences of Sexuality and Sexual Health Education of Young Women With Spina Bifida
Authors: Courtney Streur (MD), Christine Schafer (BS), Valerie Garcia, Elisabeth Quint (MD), David Sandberg (PhD), and Daniela Wittmann (PhD)
Year: 2019
Journal: The Journal of Sexual Medicine
2. Paper title: “I Tell Them What I Can Feel and How Far My Legs Can Bend”: Optimizing Sexual Satisfaction for Women With Spina Bifida
Authors: Courtney Streur (MD), Christine Schafer (BS), Valerie Garcia, Elisabeth Quint (MD), John Wiener (MD), David Sandberg (PhD), Claire Kalpakjian(PhD) qand Daniela Wittmann (PhD)
Year: 2019
Journal: The Journal of Sexual Medicine
3. Page Title: Mayo Clinic: Spina Bifida, Symptoms and Causes
Authors: Mayo Clinic Staff
Last Site Updates: 2021
Organization: Mayo Clinic
Note: Though this is not a peer reviewed academic paper, this source was verified to comply with the HONcode standard for trustworthy health information.
.jpg)



Comments